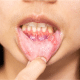
Dry Socket Explained: Managing Pain and Promoting Healing
Key Takeaways
- Dry socket is a painful dental condition that can occur following tooth extraction, potentially leading to infection and/or delayed healing.
- Professional treatment strategies such as cleaning the area, applying medicated dressings, prescribing antibiotics or rinses, and suggesting medications are used to manage dry socket pain.
- Preventive measures such as abstaining from smoking and avoiding hard foods help reduce the risk of developing dry socket after surgery.
Understanding Dry Socket and Its Consequences
Dry socket, also known as alveolar osteitis, is a painful dental condition that may occur following a tooth removed, leaving an empty tooth socket and can occur from a dry socket from a broken tooth. Although rare, untreated dry socket can lead to infection or delayed healing. This condition occurs when a blood clot fails to form or is dislodged after tooth extraction, exposing bone and nerves in the empty socket, which can lead to intense pain in the tooth socket and along the nerves of the face. In fact, dry socket is the most frequent complication associated with tooth removals, including the extraction of third molars or wisdom teeth.Developing dry socket can disrupt the proper healing process and potentially lead to infection if the dark blood clot is dislodged. The empty tooth socket exposes the underlying bone, resulting in severe pain. Fortunately, with proper treatment, a dry socket can heal without causing lasting damage, but many wonder does dry socket heal itself.Being aware of the repercussions of dry socket can guide you in taking the appropriate steps towards healing and steering clear of additional complications. A proactive approach to oral care can significantly reduce the risk of developing dry socket and ensure a smooth recovery after tooth extraction.Identifying the Signs of Dry Socket


- Severe pain
- Exposure of bone
- Swelling
- Pain may be exacerbated when exposed to cold or may not be completely alleviated by painkillers
When to Seek Dental Care
If you experience an increase in pain or the onset of new pain after tooth extraction, it is imperative to consult a dentist for accurate diagnosis and treating dry socket. Dry socket treated by a dentist can help alleviate pain and promote healing. In addition to pain, other symptoms that should prompt a dental consultation regarding dry socket include the loss of part or all of the blood clot at the tooth extraction site, pain radiating to the ear, eye, temple, or neck, and swelling of the lymph nodes.Neglecting dental care when dry socket is suspected can lead to complications such as:- Infection
- Slowed healing
- Severe pain
- Persistent bone infection
The Causes Behind Dry Socket


Risk Factors Linked to Dry Socket


- Smoking
- Oral contraceptive use
- Sucking out of a straw
- Preexisting jawbone issues
- Bottom jaw wisdom teeth extractions
Professional Treatment Strategies
Dentists typically manage dry socket by:- Cleaning the area
- Applying medicated dressings
- Prescribing antibiotics or rinses
- Suggesting medications to help reduce the likelihood of dry socket and infections
Medication and Pain Relief
For pain management of dry socket, over-the-counter pain medications, cold compresses, and prescription pain relievers are available. NSAIDs (nonsteroidal anti-inflammatory drugs) such as ibuprofen and acetaminophen are the most effective over-the-counter pain medications for dry socket. Cold compresses have been observed to be effective in managing pain from dry socket, as they can alleviate pain and reduce swelling. It is advised to use a cold pack or a cooled tea bag as a cold compress.Prescription pain relievers such as non-steroidal anti-inflammatory drugs (e.g., ibuprofen) or a combination of narcotic with acetaminophen and codeine (e.g., Tylenol® 3) are typically recommended for dry socket. Typically, the pain from dry socket can be relieved within one to three days with medication.Follow-Up Care
Consistent follow-up appointments with the dentist are important for monitoring healing progress and adjusting treatment as needed. A typical follow-up visit for dry socket treatment typically includes an examination by your dentist to evaluate the healing progress and address any symptoms. Your dentist may provide guidance on how to manage your symptoms and ensure proper healing.To ensure optimal treatment, it is advised to follow the guidance of your dental professional for the appropriate follow-up schedule. Sticking to your scheduled appointments with your dentist or oral surgeon for dressing changes and other care is important for successful dry socket treatment.Home Care for Dry Socket Recovery


Preventive Measures to Avoid Dry Socket
To mitigate the risk of dry socket, dentists advise careful adherence to their instructions, mindful rinsing, and cessation of smoking before surgery. These instructions may include:- Abstaining from smoking
- Avoiding the use of straws
- Avoiding consumption of hard foods
- Limiting excessive rinsing of the mouth
- Brushing the teeth gently around the extraction site
- Abstaining from carbonated beverages
Dry Socket Decoded: Navigating the Path to Pain Alleviation and Healing Harmony
Frequently Asked Questions (FAQ’s)
Will dry socket heal on its own?
Yes, dry sockets can heal on their own in most cases. However, since the pain associated with it can be moderate to severe, it’s best to visit your dentist for treatment to alleviate discomfort more quickly.
How do I know if I’ve got a dry socket?
If you have a severe, persistent, throbbing pain in the area of your tooth extraction 2-4 days after surgery, accompanied by bad breath and a slight fever, you may have dry socket. It will also look like an empty hole in your gums with a whitish layer at the bottom.
What is the fastest way to get rid of a dry socket?
To get fast relief from dry socket, clove oil, salt water, hot and cold compresses, honey, NSAIDs, turmeric, green and black teas, and aloe vera can all be used.
How do you treat a dry socket?
To treat a dry socket, your dentist may suggest flushing the socket out and dressing it with medicine. In addition, they will likely recommend taking pain medication and performing self-care, such as using salt water rinses and ice packs to relieve discomfort.
What is a dry socket?
Dry socket is a painful condition that occurs after tooth extraction and can leave an empty tooth socket. It is a commonly encountered complication of tooth extractions, causing throbbing pain for several days.