What Happens During a Dental Cleaning
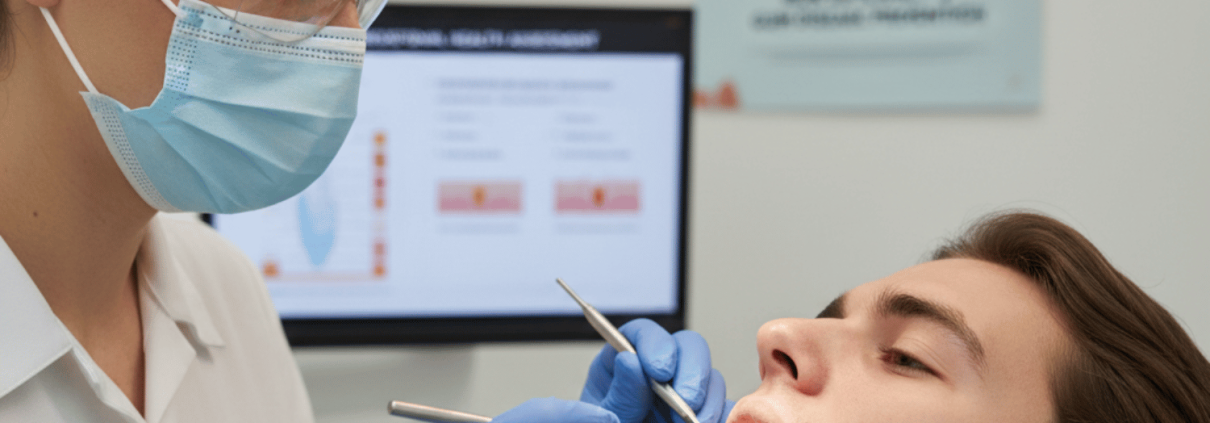
If you’ve ever wondered what actually takes place when you sit down in the dental chair, you’re not alone. Many patients, whether visiting for the first time or returning after a long gap, feel uncertain about the teeth cleaning process. At Today’s Dental in Omaha, we believe that understanding each step helps you feel more comfortable and confident during your visit.

Key Takeaways
- A routine dental cleaning at Today’s Dental in Omaha typically takes 30–60 minutes and is designed to be comfortable, thorough, and highly preventive.
- Your cleaning appointment usually includes a dental exam, removal of plaque and tartar, polishing, professional flossing, and an optional fluoride treatment to strengthen enamel.
- Professional cleanings remove hardened tartar buildup and bacteria that regular brushing and flossing at home simply cannot reach, significantly reducing your risk of cavities and gum disease.
- Most patients benefit from cleanings twice a year, while those with gingivitis or periodontal disease may need more frequent visits every three to four months.
- If you feel nervous about dental visits, our team offers gentle techniques, clear explanations at every step, and comfort options to help you relax throughout your appointment.
What Is a Professional Dental Cleaning?
A professional teeth cleaning, also called prophylaxis, is a preventive procedure performed by a dental hygienist or dentist to remove plaque, tartar, and stains from your teeth and along the gum line. Unlike daily brushing, this specialized treatment addresses buildup that has hardened over time and requires special instruments to remove safely.
At Today’s Dental in Omaha, a standard cleaning is usually combined with a comprehensive dental exam. This means you receive both prevention and early detection of potential problems in a single, efficient visit. Professional cleanings reach areas that your toothbrush and floss cannot access effectively, particularly between teeth, below the gum line, and on the surfaces of back molars.
Routine cleanings are recommended for both adults and children. Pediatric guidelines suggest a first dental visit around age one, with professional cleanings beginning once several teeth have erupted. As a local Omaha provider, Today’s Dental uses modern instruments and gentle techniques to make every cleaning thorough yet comfortable for patients of all ages.
Step-by-Step: What Happens During a Dental Cleaning Visit
While specific details may vary slightly by patient, most cleanings at Today’s Dental follow a predictable sequence. Knowing what to expect can help ease anxiety and allow you to focus on the positive outcomes of preventive care.
Throughout your visit, your hygienist will explain each step, check in about sensitivity, and adjust their approach as needed. A standard cleaning and exam typically takes about 45 minutes to one hour. Common instruments you may see include a small mirror for visualization, hand scalers for precision work, an ultrasonic cleaner for efficient tartar removal, and a polishing handpiece for that smooth, fresh finish.
Initial Check-In and Medical History Review
When you arrive, our front desk team will greet you and help you complete or update your medical and dental history. We’ll also verify your insurance information before your cleaning begins. This step ensures we have the most current picture of your health.
The team at Today’s Dental reviews your medications, health conditions such as diabetes, heart disease, or pregnancy, and any recent changes. These factors can affect gum health and influence treatment recommendations. This is also the perfect time to mention any dental anxiety, jaw issues, or past negative experiences so we can adapt your visit accordingly. Questions are always welcome from the very start.
Oral Exam and X-Rays (When Needed)
Your dental hygienist begins the clinical portion by using a small mirror to examine your teeth, gums, and soft tissues. They’re looking for signs of plaque buildup, inflamed gums, chipped teeth, or obvious cavities that need attention.
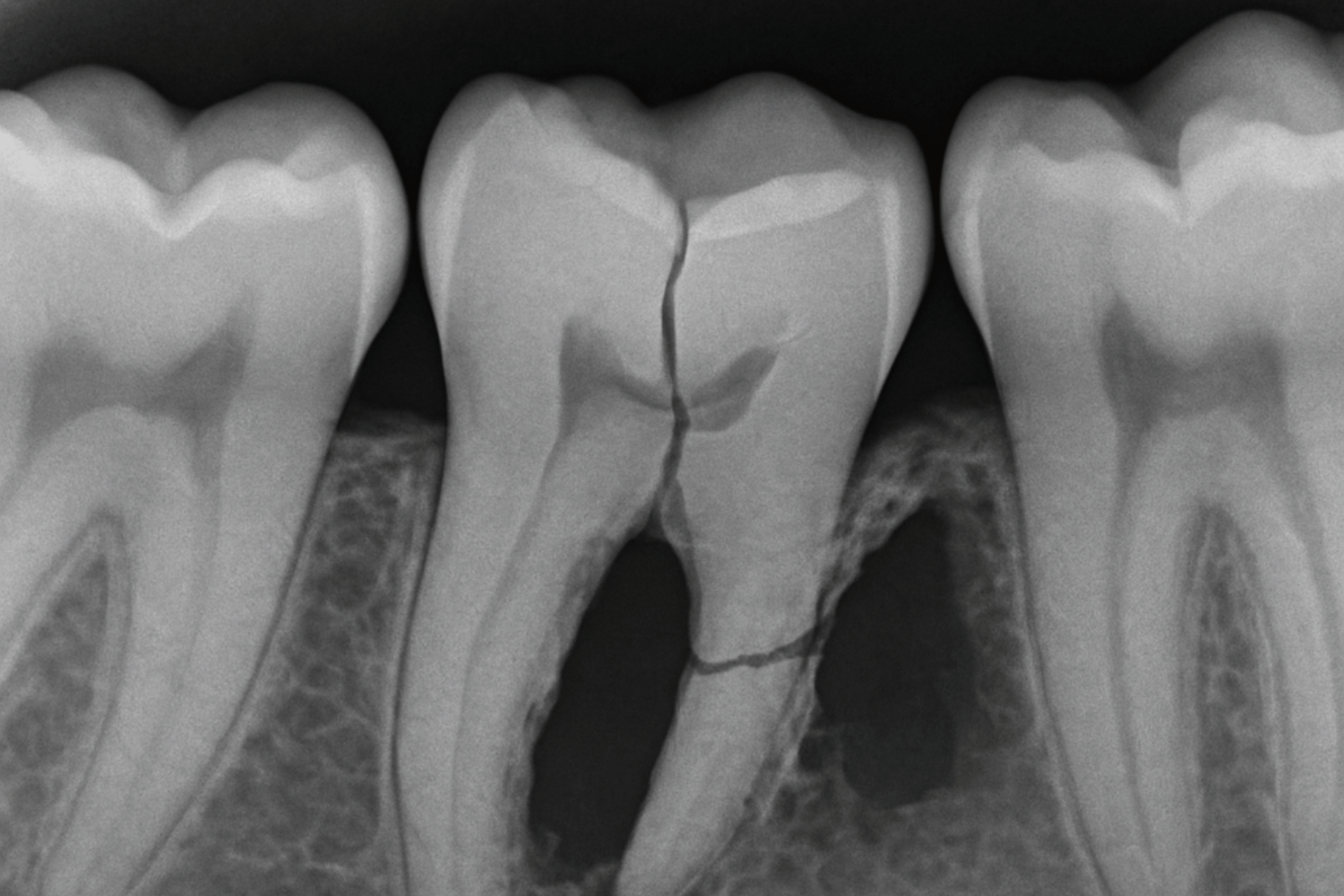
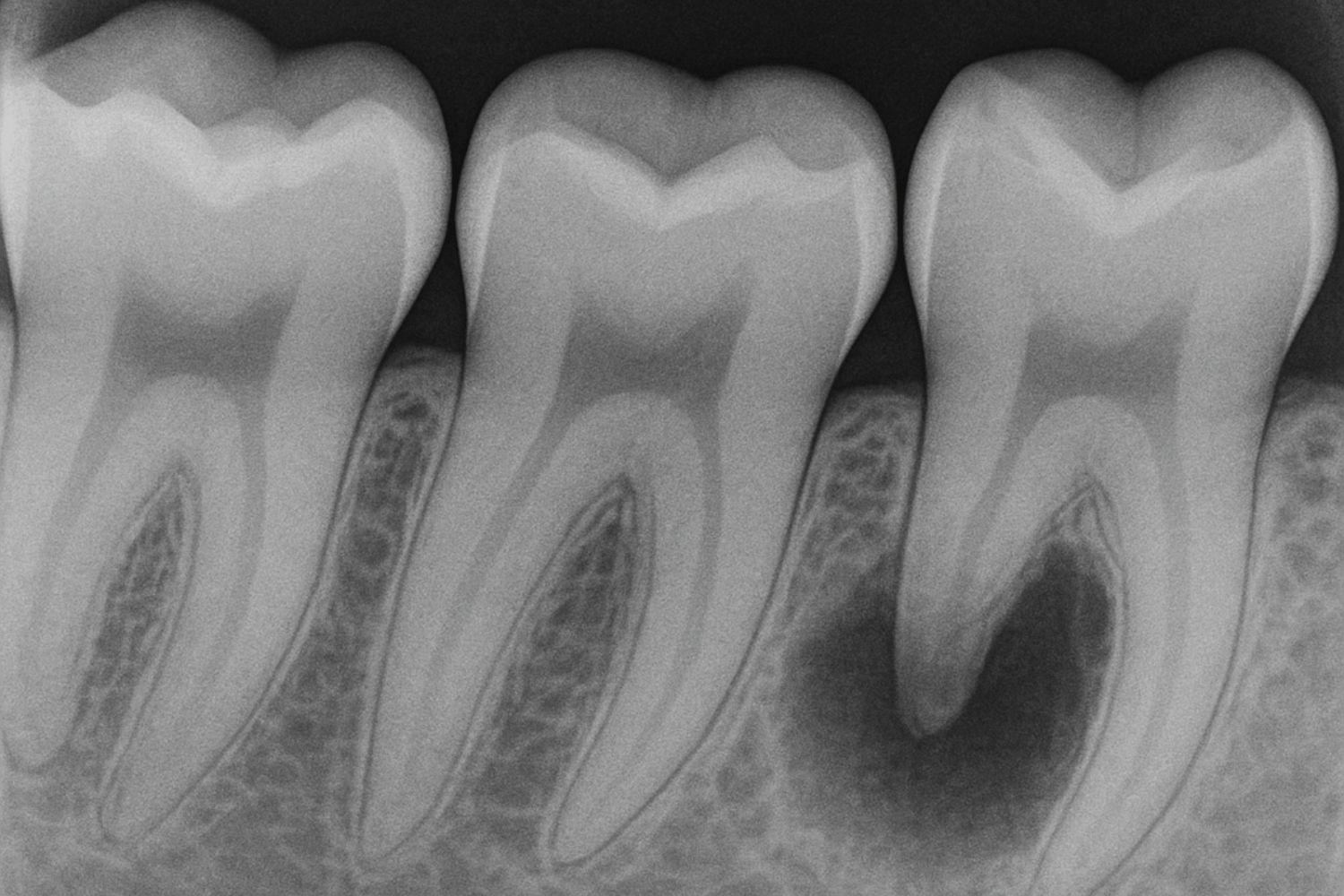
X rays may be taken once a year or as needed to detect:
- Decay between teeth that isn’t visible to the eye
- Bone loss around tooth roots
- Infections below the gum line
- Other oral health issues not apparent during visual examination
For new patients at Today’s Dental, a more comprehensive evaluation often includes checking your jaw joint (temporomandibular joint), bite alignment, and an oral cancer screening. Any concerns spotted by the hygienist will be documented and discussed with the dentist, who performs a final exam after your cleaning is complete.
Removing Plaque and Tartar (Scaling)
Scaling is the core procedure where your hygienist uses specialized instruments to remove plaque and tartar from the surfaces of your teeth and along the gum line. Plaque is the soft, sticky film of bacteria that forms constantly on teeth. When plaque isn’t removed through regular brushing and flossing, it hardens into tartar (calculus) that only professional instruments can remove.
The hygienist uses a combination of:
- Ultrasonic scaler: Vibrates at high frequency with water spray to loosen and flush away larger deposits
- Hand scalers: Hook-shaped instruments for precise, manual removal of remaining tartar
- Curettes: Specialized instruments for cleaning below the gum line when needed
The time spent on scaling depends on how much buildup is present. Patients with more tartar may notice more scraping sounds, but most patients feel only mild pressure rather than pain. At Today’s Dental, we encourage you to raise your hand if you feel any discomfort; we can adjust pressure, apply topical numbing gel, or take short breaks as needed.
This careful scaling process helps remove bacteria responsible for bad breath, tooth decay, and gum disease progression.
Polishing to Smooth and Shine Teeth
After scaling, your hygienist uses a small rotating rubber cup or brush attached to a motorized handpiece. This cup holds a mildly gritty polishing paste called prophylaxis paste that cleans and smooths tooth surfaces.
Polishing accomplishes several things:
- Removes any remaining plaque film
- Buffs away surface stains from coffee, tea, red wine, or tobacco
- Creates a smooth surface that makes it harder for new plaque to stick
- Leaves your teeth feeling slick and refreshed
While this step sounds noisy, most patients find it comfortable—similar to the sensation of using a high powered electric brush at home. At Today’s Dental, we may use different polish grits depending on your stain level and whether you have sensitive teeth, tailoring the treatment to your individual needs.

Professional Flossing Between Teeth
Your hygienist then flosses carefully between each tooth and along the gum line. This step removes any leftover debris and allows the hygienist to check for bleeding gums or tight contacts between teeth.
Bleeding during professional flossing can be an early sign of gingivitis or gum inflammation. If this happens, your hygienist will discuss it with you and may recommend ways to improve your home care routine.
Even if you floss regularly at home, this professional flossing can reveal areas you might frequently miss. Your hygienist may share practical tips on:
- Proper flossing technique to maximize effectiveness
- Alternative tools like water flossers or interdental brushes
- How often to replace your floss or flossing tools
Rinsing and Optional Fluoride Treatment
After polishing and flossing, you’ll rinse to wash away paste, loosened plaque, and debris. A small suction device helps keep you comfortable throughout this process.
A fluoride treatment is an optional but commonly recommended final step. Fluoride strengthens tooth enamel and helps prevent cavities by making enamel more resistant to acid attacks from bacteria. The treatment involves applying a flavored gel, foam, or varnish to your teeth.
At Today’s Dental, fluoride is especially recommended for:
- Children and teenagers
- Adults wearing braces or other orthodontic appliances
- Patients at higher risk for decay
- Those with dry mouth or other oral health issues
The application itself takes only a few minutes. You may be asked to avoid eating or drinking for about 30 minutes afterward to let the fluoride fully absorb into your enamel.
Final Dentist Exam and Treatment Recommendations
Once the cleaning is complete, the dentist reviews your X rays, visually inspects your teeth and gums, and confirms the hygienist’s findings. This comprehensive dental exam looks for:
- Cavities requiring treatment
- Cracked or worn fillings
- Gum recession
- Signs of oral cancer
- Changes since your last visit
This is the ideal time to ask questions about sensitivity, cosmetic concerns like professional whitening, or any future restorative work you’ve been considering. Our team takes a transparent approach, explaining findings clearly and discussing all your options.
Before checkout, we’ll help schedule your next cleaning and any follow-up treatment. We can also provide written instructions for aftercare if needed.
Types of Dental Cleanings You Might Receive
Not all cleanings are identical. The type recommended for you depends on your gum health, plaque levels, and history of gum disease. At Today’s Dental, we offer preventive cleanings, gingivitis-focused cleanings, and deeper therapeutic cleanings for periodontal disease.
Your hygienist and dentist decide together which cleaning is appropriate after examining your gums and reviewing X rays. Even deep cleanings are common, routine procedures designed to control infection and protect teeth from loss.
Regular Preventive Cleaning
A preventive cleaning is the standard visit recommended approximately twice a year for patients with healthy teeth and gums and minimal tartar buildup. This cleaning focuses on removing plaque, light tartar, and stains primarily above the gum line and slightly below where accessible.
Many Omaha patients with good home care, no gum disease, and no major medical risk factors stay on this six-month schedule. Regular preventive cleanings combined with consistent brushing and flossing at home help prevent cavities and avoid more complex, costly dental care later.
Gingivitis Cleaning
Gingivitis is early-stage gum disease, often marked by red, swollen, or bleeding gums without permanent bone loss visible on X rays. A gingivitis cleaning is more focused and may take longer than a standard preventive cleaning.
This treatment targets tartar and plaque along and just under the gum line where gum inflammation is present. The hygienist may recommend more frequent cleanings, for example, every three to four months temporarily, until your gums return to health.
The good news: with consistent professional cleanings and improved oral hygiene at home, gingivitis can usually be reversed. At Today’s Dental, we work with patients to develop personalized plans for restoring gum health.
Deep Cleaning (Scaling and Root Planing)
Deep cleaning, or scaling and root planing, is a therapeutic procedure for moderate to advanced gum disease (periodontitis). This treatment becomes necessary when pockets between teeth and gums have become deeper, allowing bacteria to accumulate below the gum line near tooth roots.
The process typically involves:
- Numbing the treatment area for comfort
- Thoroughly cleaning below the gum line to gently remove plaque and tartar
- Smoothing root surfaces (root planing) so bacteria cannot easily reattach
Deep cleanings are usually performed in sections, for example, treating the right side of your mouth first, then the left side at a subsequent visit. Follow-up maintenance cleanings every three to four months are often recommended.
While periodontal disease cannot be fully “cured,” regular maintenance cleanings at Today’s Dental can keep it controlled and help preserve your teeth for years to come.
How Long Does a Dental Cleaning Take?
A typical preventive cleaning with an exam at Today’s Dental usually takes about 30–60 minutes, depending on tartar buildup, whether X rays are needed, and your individual needs.
Typical durations for cleaning types:
- Preventive cleaning + exam: 30–60 minutes
- Gingivitis cleaning: 45–75 minutes
- Deep cleaning (per quadrant): 60–90 minutes
First-time patients or those who haven’t had a cleaning in several years should allow closer to an hour for a thorough evaluation and discussion. Gingivitis cleanings and deep cleanings may be scheduled for longer visits or split into multiple appointments for your comfort.
We understand that busy Omaha patients have demanding schedules. Our office works to stay on time and can help plan appointments around your work or school commitments.
How Often Should You Get a Dental Cleaning?
The American Dental Association recommends that most patients should visit the dentist for a professional cleaning and exam about twice a year. This schedule works well for many people and helps maintain optimal oral health.
However, some patients benefit from a custom schedule based on individual risk factors:
- Gum disease history: More frequent visits to prevent progression
- Smoking or tobacco use: Increased risk of periodontal disease
- Diabetes: Can affect gum health and healing
- Dry mouth: Reduced saliva increases cavity risk
- Pregnancy: Hormonal changes affect gum sensitivity
- History of frequent cavities: May need additional monitoring
Patients with periodontitis often return every three to four months for periodontal maintenance cleanings. At Today’s Dental, we use clinical findings, such as pocket measurements, X ray results, and bleeding points, to determine the right frequency for you. Dentists recommend personalized schedules based on your unique situation, not just a one-size-fits-all approach.
We encourage you to ask your hygienist directly what interval is best and why. Understanding the reasoning behind your recommended schedule helps you take ownership of your dental care.
Benefits of Regular Dental Cleanings
Regular dental cleanings do far more than make teeth feel smooth—they’re a cornerstone of long-term oral and overall health. Professional cleanings provide benefits that extend well beyond the dental chair.
Key benefits include:
- Fewer cavities: Removing plaque and tartar eliminates the bacteria that cause tooth decay
- Lower risk of gum disease: Cleanings prevent gum disease from developing or progressing
- Fresher breath: Professional removal of bacteria reduces bad breath at its source
- Early problem detection: Small issues like tiny cavities can be caught before they become bigger dental problems requiring crowns or root canals
- Brighter smile: Polishing removes surface stains, keeping your smile vibrant
- Better overall health: Research continues to explore connections between oral health and systemic conditions
At Today’s Dental, routine cleanings are also a chance to update you on home-care techniques and discuss any cosmetic goals you might have. We see these visits as an opportunity for education and partnership in your health journey.
Consider this: catching a small cavity early might mean a simple filling rather than an expensive crown or root canal later. Consistent cleanings lead to reduced long-term dental costs and less invasive treatment over your lifetime. That’s prevention working for you.


Possible Side Effects and How to Stay Comfortable
Routine cleanings are very safe procedures, but some patients may experience temporary effects afterward. Understanding what’s normal can help you feel prepared.
Common temporary effects:
- Mild tooth sensitivity, especially to hot or cold
- Slight gum soreness where tartar was removed
- Minor bleeding, particularly if gums were inflamed
These symptoms usually resolve within a day or two, especially if you follow aftercare advice from your dental team.
Comfort tips after your cleaning:
- Take over-the-counter pain relievers like ibuprofen if medically appropriate
- Avoid very hot or cold foods for a few hours
- Use a soft-bristled toothbrush for a day or two
- Consider special toothpaste designed for sensitive teeth if sensitivity persists
For anxious patients, Today’s Dental offers additional comfort measures. We can use topical numbing gel, adjust our technique for gentler cleaning, or break appointments into shorter visits. Most patients experience only mild pressure and scraping rather than actual pain.
Persistent pain, swelling, or heavy bleeding after a cleaning is not typical. If you experience these symptoms, please call our office promptly so we can help.
Aftercare: Taking Care of Your Smile Between Cleanings
What you do at home between visits is just as important as the professional cleaning itself. Consistent oral hygiene habits extend the benefits of your cleaning and protect your healthy teeth between appointments.
Daily care essentials:
- Brush twice daily with fluoride toothpaste for two full minutes, focusing on the gum line and back teeth where plaque builds up fastest
- Floss daily or use interdental cleaners to remove bacteria and debris from between teeth where toothbrush bristles cannot reach
- Consider additional instruments like antimicrobial mouthwash, electric toothbrushes, or water flossers—ask your hygienist which options fit your specific needs
Lifestyle considerations:
- Limit frequent sugary snacks and acidic drinks to reduce enamel erosion and cavity risk
- Drink plenty of water throughout the day to maintain saliva production
- Replace your toothbrush every three to four months or sooner if bristles are frayed
Before leaving Today’s Dental, schedule your next preventive visit. This simple step helps ensure your cleanings stay on track without long gaps that allow problems to develop. Traditional methods of regular brushing combined with professional care create the foundation for a healthier smile that lasts.
FAQs
Does a dental cleaning hurt?
Most patients feel only mild pressure and scraping during a standard cleaning, not actual pain. Those with sensitive teeth or inflamed gums may notice brief moments of discomfort, particularly during scaling around tender areas.
At Today’s Dental, we can use topical numbing gel, gentler techniques, and scheduled breaks to keep anxious or sensitive patients comfortable throughout their visit. The most important thing is to communicate with your hygienist, so please raise your hand or speak up right away if anything feels too sharp or intense. We’ll adjust our approach immediately.
How much does a dental cleaning cost, and is it covered by insurance?
Fees vary based on the type of cleaning needed (preventive versus deep cleaning) and whether X rays or fluoride treatment are included in your visit.
Many dental insurance plans cover routine preventive cleanings and exams at or close to 100% twice a year, sometimes with a small copay. This makes regular cleanings one of the most accessible forms of preventive care available.
If you don’t have dental insurance, please ask Today’s Dental about current fees, payment options, and any in-office savings programs or financing arrangements we offer. We believe cost should never prevent someone from receiving essential dental care.
When should children start getting dental cleanings?
Professional guidelines recommend a first dental visit by age one, with cleanings beginning once several teeth have erupted and the child can comfortably sit for an examination.
At Today’s Dental, we take extra time with young patients, using child-friendly language and a gentle approach to build positive associations with dental care. This reduces fear and establishes healthy habits early.
Regular teeth cleanings in childhood help prevent early cavities and teach good brushing and flossing skills that last into adulthood. Early positive experiences at the dentist often translate to better oral health throughout life.
What if I’m afraid of the dentist or embarrassed about my teeth?
Dental anxiety and embarrassment are far more common than most people realize and our team at Today’s Dental is trained to be completely nonjudgmental and supportive. You are never alone in these feelings.
When scheduling your appointment, please mention any fears or concerns. This allows us to plan extra time and comfort measures, such as slower pacing, clear explanations before each step, and frequent check-ins during your visit.
The goal of your cleaning is to improve your health, not to judge. Even if it has been many years since your last visit, it’s never too late to start fresh. We’re here to help you move forward, not look back.
Can I eat or drink right after my cleaning?
You can usually eat and drink immediately after a standard cleaning. However, you may want to avoid very sticky or heavily dyed foods for a few hours to maintain that fresh, clean feeling.
If a fluoride treatment or other topical medication was applied, you’ll typically be asked to wait about 30 minutes before eating or drinking. This waiting period allows the fluoride to fully absorb into your enamel for maximum benefit.
Your hygienist or dentist at Today’s Dental will provide specific post-visit instructions based on your treatment. Following these guidelines helps ensure you get the best possible results from your cleaning.